Here we go again. We thought we were done with the COVID-19 epidemic which changed the history of planet earth. But now, we have a new enemy. A Monkeypox outbreak is on the way.
It’s nothing new though. The virus has existed and infected people for more than a hundred years. The reason it didn’t ring any alarm bells was that Monkeypox was more common in animals than in humans.
Humans do get infected by it, but it does not spread that quickly. However, the variations, recently discovered in several countries including the USA and the UK, have shown evidence of a widespread epidemic waiting to happen.
What is Monkeypox?
The Monkeypox virus (MPXV) is a relative of Smallpox. It belongs to a family called Poxviridae having the genus ‘Orthopoxvirus’. There are two distinct genetic variations of Monkeypox– One found in Democratic Republic of Congo, Central Africa, and another in the West African region.
The Congo variation is known to be a lot more severe when it infects humans. It also transmits faster. Monkeypox has always existed in those regions, but only recently is it showing up in the other parts of the world.
What does the Monkeypox Virus Look Like?
It looks similar to any other Orthopoxvirus. We’ll discuss more in our Monkeypox Virology article, but for now, it has an enveloped double-stranded DNA structure. The following picture shows what the virus looks like:
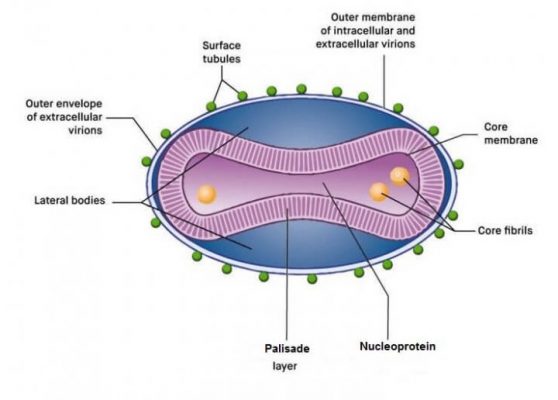
The parts of the virus include:
- Nucleoprotein Compound
- Core Fibrils
- Core Membrane
- Palisade Layer
- Outer membrane
- Outer Envelope &
- Surface Tubules that latch onto human or animal cells.
The Origin of Monkeypox
Although named Monkeypox, monkeys are not the original hosts of this virus. It was first discovered in a laboratory in Denmark. In 1958, a colony of monkeys that was kept in a testing lab first showed symptoms of the pox. It then got named ‘Monkeypox‘. No human infection was recorded at that time.
The original hosts were suspected to be rodents- Mice, rats, and guinea pigs. At that time, no research was done on what part of a rodent’s body contains the virus. However, now that an outbreak is on the way, researchers are doing a thorough investigation.
The first human to have contracted the virus was in the Democratic Republic of Congo (Formerly known as Zaire) in 1970. It was not diagnosed to be dangerous. The symptoms were very similar to Smallpox, and the patient was treated the same way, and it worked.
Furthermore, the vaccine for Smallpox also provides almost 85% resistance to the Monkeypox virus. Therefore, there was nothing to be alarmed about. The Smallpox vaccine has a slight issue. It can cause infections if the person it’s administered to has a weak immune system.
The Most Likely Cause of the Outbreak
At the end of 1980, Smallpox was almost completely eradicated and the World Health Organization (WHO) stopped the vaccination programs as it was an unnecessary health hazard. Hence, the next generation of the population was not immunized and small outbreaks of Monkeypox were noticed.
It still wasn’t that big a threat since human-to-human transmission of the virus was relatively slow and it can be treated just like we treat Smallpox. Antiviral medications exist for this disease.
Finally, the virus seemed to be contained in a particular area. Only a few people living near the wild animals in the rainforest areas of Africa were infected. The fatality rate for the more dangerous variation (Congo Clade) is about 14% and the milder one (West African Clade) is less than 1%.
However, there must be a mutation recently that has caused the virus to get transmitted to humans faster in 2022 causing this new outbreak.
How does Monkeypox get Transmitted?
What we know so far is that Monkeypox transmissions from humans to humans happen only in close proximity. Air droplets from sneezing, saliva exchange, using the same utensils (Glass, plates, and spoons), and household items such as bedsheets, blankets, and towels can cause the transmissions.
The puss from the lesions of a patient can also infect a healthy person so those who care for the patients must be extremely careful in treating the patient’s skin.
What are the Symptoms of Monkeypox?
Like most viral infections, Monkeypox symptoms begin with a fever, headache, and muscle pain. Depending on the body type, a patient may develop the symptoms 1 to 2 weeks after the exposure.
The initial symptoms are then followed by inflammation of the lymph nodes and outer skin rashes and lesions. More skin lesions are noticed on the exposed parts of the skin, especially the face and arms. It is also particularly uncomfortable if the skin rashes appear in the groin and the anal regions.
The lesions fill with yellow-white liquid (Puss). As treatments progress, they should dry up and fall away automatically. Patients are advised not to touch or scratch them regardless of how uncomfortable they are. The symptoms generally remain for 2-3 weeks.
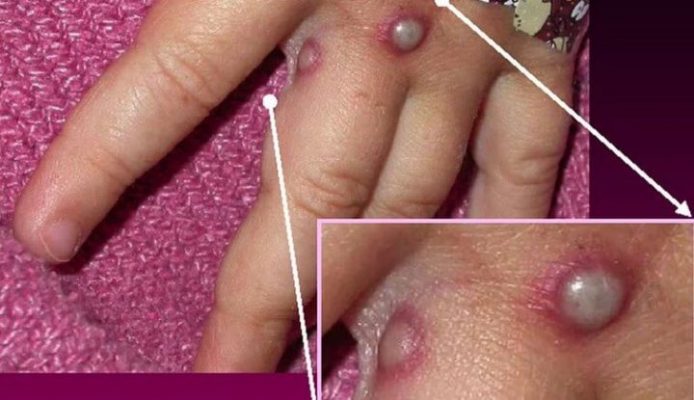
Additionally, the patient may experience diarrhea, respiratory congestion, fatigue, and blur vision. In serious cases, extreme weakness may lead to kidney failure, heart failure, and death.
Anyone displaying the symptoms or has been in close proximity to a Monkeypox patient should call the nearest health center immediately.
Should we Worry about it?
It always pays to be careful. Only in 2022, have we seen a multi-country outbreak. WHO is now very vigilant on this matter and is doing everything it can to prevent a major pandemic.
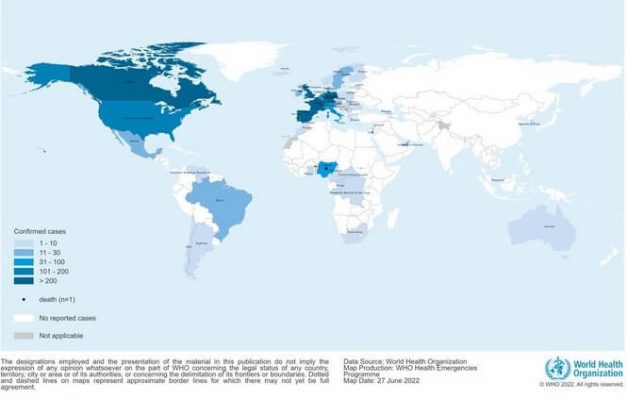
Unlike COVID-19, Monkeypox has vaccines. The treatment is also not that difficult. In most cases, the disease goes away automatically. An average healthy person needs not to worry.
Very young babies and the elderly, however, may be at risk. Babies have not developed their immune system yet and the elderly have a weakened one. Antiviral medications specially designed for Smallpox work for Monkeypox as well.
In general, no treatment is required except some analgesics to reduce fever and swelling. Acetaminophen, Ibuprofen, or aspirin will do that job. In several of our next articles, we shall discuss home treatments and medications for Monkeypox.
There will also be live updates on the world situation on this matter. For more information, check out our Monkeypox FAQ.
Share this:
- Share on X (Opens in new window) X
- Share on Facebook (Opens in new window) Facebook
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Share on Tumblr (Opens in new window) Tumblr
- Print (Opens in new window) Print

